Maintain full control with deployment in your own cloud infrastructure, ensuring the highest level of data security and privacy.
Fully integrates with your existing systems, including CRMs, ERPs, and other business platforms, ensuring seamless workflows and unified data management across all operations.
Tailored to fit your needs, because every company is unique. Our AI adapts seamlessly to your processes.
We continuously monitors our AI in your production environment, evaluating performance, detecting drift, spotting errors, and ensuring accuracy doesn’t degrade over time.
Claims47 enhances efficiency, reduces manual effort, and accelerates claim resolution using AI-driven data extraction, fraud detection, and intelligent decision-making. When combined with DocFraud47, DocProc47, and DocsTans47, Claims47 delivers an end-to-end AI-powered claims management system, reducing processing time from weeks to minutes, cutting costs, and improving customer satisfaction.
Enables Global Operations with Multilingual Support and Currency Conversion
Reduces Manual Effort Through Automation and AI-Powered Data Extraction

Enhances Customer Satisfaction with Faster Claim Resolutions

Scales Seamlessly to Handle Growing Claims Volumes
Reduces Fraud Risk by Detecting Document Anomalies Early

Ensures Accurate Provider Assignments and Coverage Validation
Streamlines Data Handling with Multi-Format Document Processing

Delivers Actionable Business Insights Through Comprehensive Data Reporting
Leverages advanced AI-powered OCR to extract key information from physical documents like PDFs and screenshots, accurately capturing complex layouts and tables. The data is then normalized and standardized, ensuring consistent formats (e.g., dates, currencies) and mapping unstructured terms to standardized fields. This enables seamless integration into core systems like CRMs for further processing.
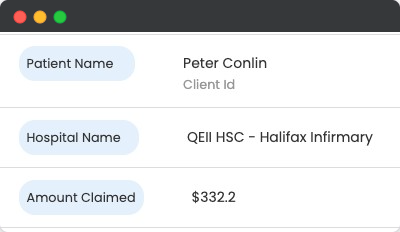

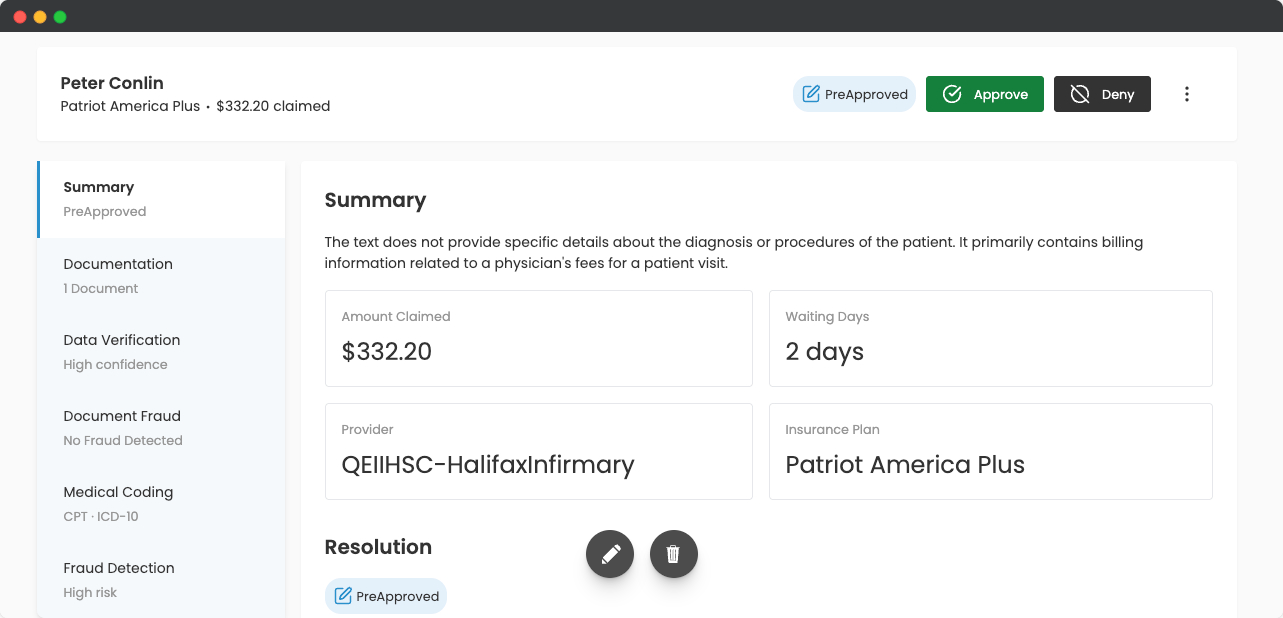
Uses AI to quickly and accurately summarize claims reports, extracting key details and providing concise overviews. It helps streamline decision-making by delivering only the most relevant information for claims processing.
Leverages AI to identify fraudulent modifications in documents, such as altered invoice amounts or falsified details. AI-driven pixel-level analysis detects tampered areas in scanned documents, while autoencoder models flag anomalies by learning the typical structure of legitimate documents. Additionally, it compares documents against historical records or templates to spot inconsistencies and potential fraud, and applies rules like dates validation.

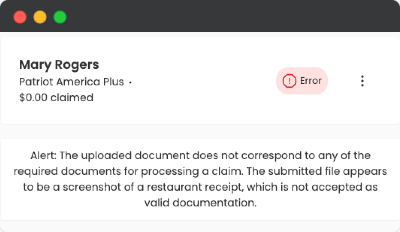
Ensures that the right documents are uploaded for each claim. Using AI-powered analysis, it automatically classifies documents like invoices, medical reports, bank statements or national IDs, verifying that they match the required types for the claim. If incorrect or missing documents are detected, the system alerts the user, ensuring that claims are processed with the correct information from the start. This reduces errors and speeds up the approval process.
Ensures accuracy by validating extracted data against internal databases, such as matching provider names with hospitals. AI-powered fuzzy matching technique allows the system to recognize and correct slight variations or typos (e.g., 'John's Medical Center' vs. 'John Med Center'), ensuring accurate matches and seamless data integration.
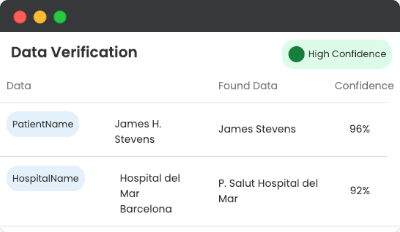
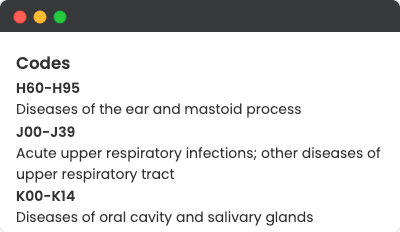
Automatically maps medical terms to standardized codes (e.g., ICD-10-CM, CPT), ensuring precise data representation with minimal manual intervention. This feature supports consistent coding across multiple standards like SNOMED and provides automated suggestions to assist coders, improving both speed and accuracy.
Automatically converts invoice values into a predefined currency using real-time exchange rates. AI detects and normalizes currencies from symbols, abbreviations, and contextual clues, ensuring accurate conversions even in ambiguous cases. With built-in exchange rate anomaly detection, it flags unusual rates, preventing errors or fraud. This solution streamlines international claims, reduces administrative overhead, and ensures transparent, accurate transactions.
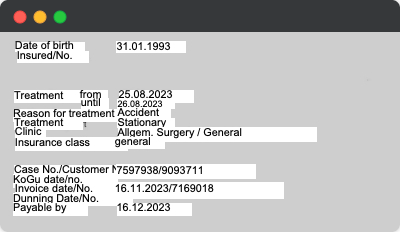
Automatically converts key claim fields, such as treatment or maneuvers descriptions, into the destination language set in the system. AI-powered language translation ensures accuracy, preserving critical medical, legal and technical terminology. With customizable field selection, dynamic language detection, and support for multiple languages, the system streamlines international claims processing while maintaining terminology consistency through industry-specific glossaries.
Leverages AI to analyze claim patterns and compare them against vast historical data to identify anomalies and inconsistencies. It flags suspicious claims early, ensuring proactive fraud prevention without delaying legitimate claims. This data-driven approach reduces investigation costs, adapts to emerging fraud tactics, and helps protect the insurer's bottom line.
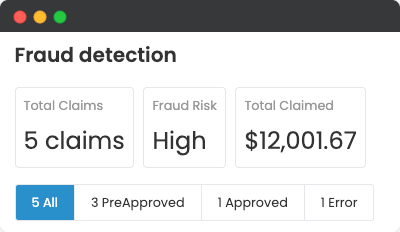

Our AI acts as an AI Agent and with all the collected information, plus insurance policies, VoB (Verification of Benefits) or business rules automates the validation of claim data. It checks coverage eligibility and assigns statuses such as approved, denied, or requiring manual review, ensuring fast and accurate claim processing. This component reduces operational costs, enhances compliance, and minimizes manual intervention, enabling adjusters to focus on complex cases.
Automates the creation and delivery of personalized messages to claimants at every stage of the claims process. AI-powered GenAI drafts contextually relevant messages based on claim status, claimant details, and business rules, ensuring timely and accurate communication via email, SMS, or push notifications.
"Working with M47 AI helped us transform a slow, manual process into something faster and more consistent. The AI system they helped us build assists our teams in reviewing medical forms, reducing human workload by up to 80%, while ensuring that final decisions remain in expert hands and fully comply with regulatory standards."

Claims47 is an AI-powered solution designed to transform how insurance companies manage claims. It automates and optimizes the full claims lifecycle, reducing processing time, improving accuracy, and enhancing the customer experience.
Claims47 is built for insurance providers, third-party administrators, and claims handling teams that want to streamline operations, reduce costs, and improve claim turnaround time. It is suitable for organizations of all sizes and adaptable to different types of insurance.
Clients typically experience:
- Shortened insurance claims processing cycles (from weeks to minutes)
- Lower operational costs
- Enhanced claims fraud prevention
- Improved customer satisfaction (increased NPS)
- Scalable performance as claim volumes grow
Yes. Claims47 is designed to work seamlessly with your existing infrastructure, including CRMs (like Salesforce, Hubspot or Microsfot Dynamics), ERPs, and other platforms. Integration is straightforward and supported by M47’s technical team to ensure a smooth transition.
Absolutely. Claims47 is customizable and flexible, allowing it to conform to your workflows, rules, and operational preferences. It is built to fit into your organization rather than forcing you to adapt to a rigid system.
The solution can be deployed within your own cloud environment, giving you full control over data management. It supports industry-standard privacy and security protocols to ensure your sensitive information remains protected at all times.
Yes. Claims47 is designed to support global insurance operations, including multilingual claims handling and currency conversions, making it ideal for international teams and customer bases.
You can reach out to the M47 team through our contact page or by email at info@m47labs.com. We offer consultations to understand your needs and propose a tailored implementation plan.
Our SPECIALIZED AI offer a modular, customizable AI product portfolio, designed to integrate seamlessly into existing systems and adapt to specific business needs.